Well, I was waiting to have a little more news to put out this update, but as I’m trying to let go of some of my “perfectionist” feelings to have things “complete” and instead just get things done, I’m going to try to just go ahead and post what I have.
Last week we had a little craziness, as Kevin’s been having some nausea that by Wednesday night had increased in frequency and intensity. This is not a “normal” side effect for his treatment (but seeing as this is a phase one trial, that’s a pretty relative term). Regardless, after Kevin having nausea and vomiting from 6PM Wednesday night to 6AM Thursday morning, I made the command decision to bring him in to Emory to get checked out. I pretty much had to drag the guy because he told me there was some important stuff at work he needed to do that morning. He hadn’t thrown up for a few hours, so he said he was pretty sure he was better. Then he sat up in bed and threw up. And I said to him, “…And, I rest my case. We’re going.”
I am so grateful for my amazing neighborhood that we live in. If any of ya’ll are looking for a home in Atlanta, I cannot recommend Adair Park enough as an amazing place to live. It’s truly the people that make the difference. I texted my neighbor Maiya to see if she could have her adult niece come over and stay with the kids (who were still asleep) until we got back and less than a minute later, at six in the morning, she said that Angela was at the front door. Angela came in and went back to sleep in the guest bedroom till the kids got up while I spoke with the on call doctor and then we headed in to Emory.

My amazing neighbor and bestie Maiya and her niece Angela
We arrived at 7:30, which is when the doctor said that the infusion center opened, and I think he was wrong about that because the place was already packed! Luckily they brought him in right away to be seen by the triage nurse and by 8:00 Dr. Lawson’s nurse had received my middle of the night emails and was discussing necessary interventions with the infusion center staff. In another half an hour, Kevin’s blood work was done and he was getting settled into those oh so cushy vinyl lazy boys to get all filled up on fluids and the “good stuff” anti-nausea meds. I spoke with our Emory team and we decided to wait and see what the UCLA team said as far as this being some sort of adverse (or even potentially good!) indicator of his treatment and by 11:00 we were back home.
The good stuff
Kevin was feeling gobs better, and seeing as he doesn’t get paid if he’s not at work at this point, he decided to head on in. I hadn’t slept in over 24 hours, so two of my other neighbors took care of the kids through to naptime so I could get some rest. I am so grateful that Angela, Dawn, and Erica were there for us that day. I was able to focus on Kevin and care for him and then take care of myself and get the rest I needed. And because these were neighbors that my kids see on an almost daily basis, neither Jude nor Evie shed any tears over why their mommy wasn’t there when they woke up, etc. Having a community of friends within walking distance from my house is such an amazing blessing and experience that I’ve never really experienced before moving into this neighborhood. It is amazing, and incredibly useful as well!
On Friday as I was getting ready for our flight to LA for Kevin’s next infusion, I heard from Liz, the director of Kevin’s trial at UCLA. She said she’d finally spoken with Dr. Ribas and he wanted Kevin to get a brain MRI as soon as possible, before flying to LA if possible. In that moment my heart stopped. She didn’t have to say it, I knew what that meant. I remember sitting in the van, parked in the driveway, thinking that if it wall went downhill from here, that this was the moment I would look back and remember as the start of the next chapter. I took a deep breath, closed my eyes, and tried to figure out what I should be doing. What was going to happen next? What do I worry about? What do I find peace in? I felt lost and frenzied and frozen all at the same time. Finally, somehow, I started to put the pieces together of what I needed to be doing. First I contacted Emory and tried to see if they could even get an MRI scheduled for today. I realized it was unlikely we’d be able to make our flight, so then I got on the phone with Southwest and very sweetly finessed a reservations agent to see if we could get our flights rescheduled to the next day. Oh Karen, bless her! She not only got our flight rescheduled, but got us on a non-stop and didn’t charge my friend’s account any extra miles even though the change was totally last minute. Southwest, you are amazing!

Finally on our way… Southwest rocks!
Only then did I call my poor husband to tell him that his entire day’s schedule was changing. I kept working out details and making changed plans with the folks we were staying with, visiting, etc. in LA. And then of course, wouldn’t you know it by 4:00 our Emory team called me and said they’d tried everything and everywhere but they just weren’t going to be able to get Kevin in for an MRI that day. THEN, I had to call Liz at UCLA back, tell her that, and see if she could get one scheduled at UCLA for Monday. THEN, I was ready to just pass out from exhaustion. It’s after days like these that I really wished I drank. Or frankly, it’s probably a good thing I don’t drink, because I’d become an alcoholic!
We did our best to put our worries out of our mind for the weekend and focus on enjoying time with family. We visited Kevin’s mom’s cousin’s family down in San Diego and had just the best time catching up, snuggling with new babies and just spending quality time together. The rest of the trip was spent at Kevin’s cousin Claudia’s house, which is just down the street from UCLA (how convenient!)

Fun girls’ night with Kevin’s mom’s cousin’s, sons’ wives. So that makes us… I have no idea, except family!
Tuesday was UCLA day and wouldn’t you know it, they were totally behind with his bloodwork which pushed everything else behind. Again I quickly realized we were NOT going to make our 3:30 flight, which was Southwest’s last flight of the day, so MORE calling and finagling and sweet talking to get the flight changed. And just when I’d gotten it worked out and approved by a supervisor, my stupid phone hung up on sweet Mary! Noooooo!!!!! I seriously need a new phone, this one has just been through one too many bouts with a toddler and randomly hangs up on people, has wild volume swings up and down and is just a downright bipolar phone. And in that moment it felt like my phone was kicking me in the face! Argh!!! I tried again and this time just barely got someone to be willing to switch the flight for us without charging a boatload of points. All told I’d been on the phone with Southwest for over an hour trying to get this all done because of some stupid labs being delayed!
For the love of Pete, how much bloodwork do we need?!
Kevin met with Dr. Ribas before his infusion and we discussed the nausea that he’d had in the previous few weeks, culminating in his hospital visit last week. Dr. Ribas did NOT think that the nausea felt consistent with a brain metastasis (he would have been much sicker and not have had times of feeling well) but it was still a strange side effect. When we discussed the gassiness that seems to lead to it, he started to think that Kevin might have cancer in his gut somewhere. This is an area that would not show up on a scan very well because of how much “stuff” we have down there in the ole GI tract. This would explain SO much from the last six months. Kevin has really had a lot of nausea that has dogged him through interferon, IL-2, and now Anti-PD1. And it was never “normal” nausea and “normal” meds usually didn’t help very much. Also, the way the Anti-PD1 treatment works, it could effectively “piss off” the areas of his body that have cancer in them, like they could “flare up” when they’re being attacked, you know? So that makes perfect sense, right? Here, maybe this will help.
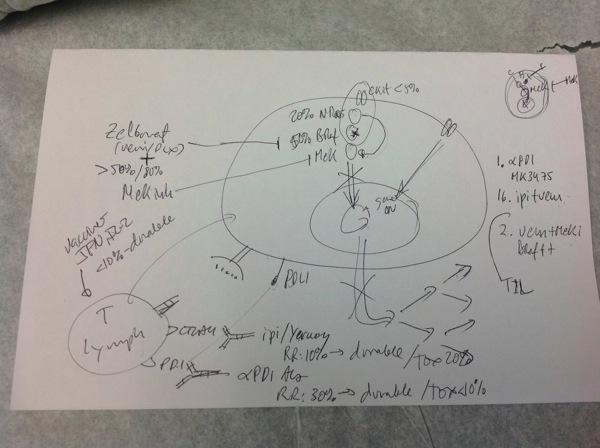
Dr. Ribas’ notes “explaining” how Anti-PD1 treatment works.
So here we are, back at Emory on a Thursday evening. Kevin is finally having the brain MRI and we ask you to join us in prayers for NO brain metastasis. But he is also having an X-ray of his abdomen and I don’t know what I really pray will come of that. Do we want them to find cancer there which would explain a lot of troubling and unexplained symptoms? In some ways that would be comforting, but still that would mean he has more cancer than we knew he had. More cancer is definitely worse than less cancer. I don’t know if it would change things with treatment or what. So I guess we just ask that you pray the God would make things work out the way they should and that things are clear to our doctors so they have wisdom in which way to proceed.
I will post as soon as we hear the results of these scans as well as the biopsy that Kevin had done on Tuesday. We are hoping that the biopsy will show that there are a higher number of fighter cells in his tumor tissue than were present at the biopsy he had before commencing treatment. This would be a good indicator that the treatment is being effective.
Kevin’s biopsy…That’s no baby on that screen
Kevin will have one more infusion before scans are done to see if there has been any progress. Thank you again dear friends and family for all of your thoughts, prayers, support, and encouragement. Even if I don’t always respond, I read every comment, email, facebook post, and text message. They warm my heart and remind me that we have not been forgotten. We are SO incredibly grateful for each and every one of you. Thank you!







































